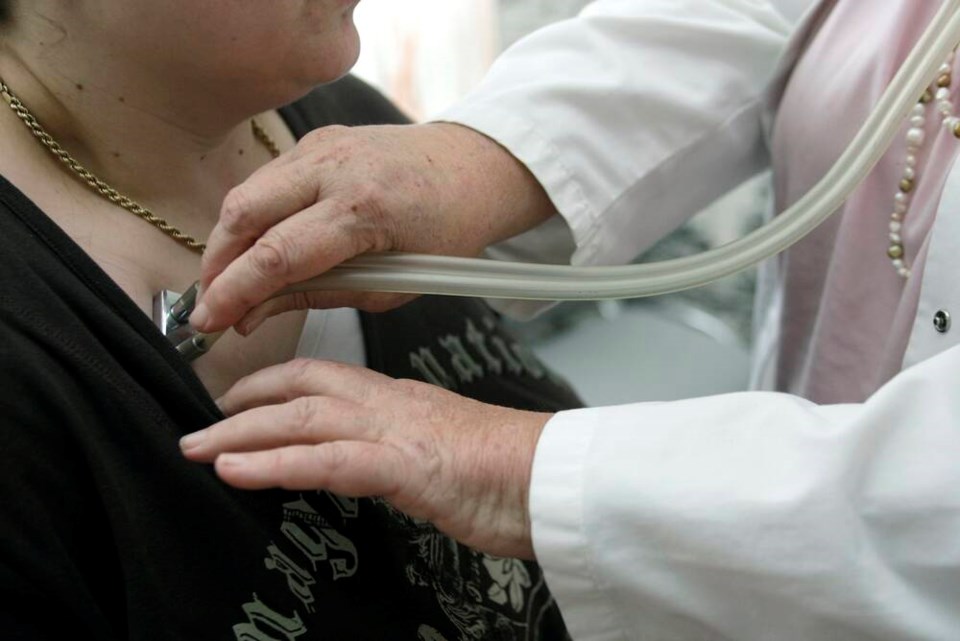
The decision to close their practice by two well-liked family physicians in View Royal has sparked heated commentary.
The two intend to give up what’s called longitudinal care, meaning personalized care for patients with whom they have an ongoing relationship. Instead, they plan to sign up with one of the tele-health companies such as Telus Health that offer distant, one-off care. That means their contact with individual patients is broken.
The husband-and-wife team cite low fee schedules as contributing to their decision. The Medical Services Plan pays just $31.62 for a patient consult. With overhead and rent to cover, this is the barest of minimums.
Many readers have written to the Times Colonist protesting what certainly appears an impossibly low scale of remuneration for an often complex consult.
However, things aren’t quite that simple. While the fee for a consult is only $31.62, consults can occur for numerous reasons, such as to order a test, report test results, write a prescription, and so on.
While estimates vary, depending on hours worked and patients seen, the average family physician in B.C. bills between $250,000 and $300,000, often higher. While overhead and administration must be paid out of this amount, that’s still quite a bit more than the $31.62 billing rate might suggest.
It would help inform this discussion if the Health Ministry were to speak out and clarify the matter.
However, money is not the only problem. Family practice has become enshrouded in paperwork, while time-consuming administrivia drive up expenses and reduce time with patients. It’s understandable that physicians are increasingly reluctant to enter this field.
The Eagle Creek doctors make that point, and the growing shortage of family physicians reinforces their complaint.
One option might be for the province to offer rent-free accommodation to family-practice clinics. And something must be done to remove the overburden of stifling regulations.
However, there is a larger issue. If Canada’s family physicians begin practising through tele-health portals, quality of care will suffer.
A distinction is needed. During the COVID outbreak, many doctors have been consulting with their patients by phone or online.
This has been beneficial, for it offers a simplified way of dealing with routine matters such as refilling prescriptions.
However, in the tele-health model discussed here, physicians sever the relationship they have with their patients.
Instead they advise and prescribe at a distance, detached from ongoing contact with their patients.
This is not family medicine in the traditional sense, since only those individuals who can get by with occasional, distant consults are treated.
If an increasing number of family physicians migrate to this form of practice, that will leave more needy patients with even fewer options.
The representative bodies who speak for our country’s physicians recently took this matter up.
A Virtual Care Task Force has been created by the Canadian Medical Association, the College of Family Physicians of Canada and the Royal College of Physicians and Surgeons of Canada.
Their key recommendation reads: “Encourage provincial and territorial governments and provincial and territorial medical associations to develop fee schedules that are revenue neutral between in-person and virtual encounters.”
This is an open invitation to family physicians to give up their practices and resort to distant medicine. Not a word is said about the importance of maintaining ongoing, face-to-face contact with patients.
Yet if nothing is done, this may very well become the future of “family” medicine — remote, disembodied and impersonal.
We cannot stand by and watch family medicine disappear.
This is an urgent matter that federal and provincial health ministers should address. Virtual medicine has a role to play as a means of strengthening and extending family practice.
But it is not, and must not be allowed to become, a substitute.