Across B.C., people are working in health care amid a global pandemic. Many cheer them from their balconies and porches each night at 7 p.m. Often in his daily briefings, B.C. Health Minister Adrian Dix takes a moment to thank them, not just the physicians and nurses, but all the allied health-care workers — those who work in seniors care homes, care aids and janitors.
Here, you’ll meet a handful of those workers at Royal Jubilee Hospital and hear about their first brushes with the virus. Some common themes emerge from their stories. In the early days, they would worry about bringing COVID-19 home to their families. Some self-isolated; some couldn’t bear that. Many have found the transition to wearing protective equipment all day difficult and feel the pain of patients who can’t have visitors. Mostly, says the head of the emergency and critical-care departments for Island Health, these workers have carried on “humbly” and “bravely” and put their patients before their fears.
Royal Jubilee is one of two COVID-19 designated hospitals on Vancouver Island (the other is in Nanaimo). It has three critical-care units: the intensive care unit, with 11 beds for patients typically needing multiple organ support, and two others, with eight beds each, for coronary care.
There are two negative-pressure rooms in the ICU for procedures that cause the COVID-19 virus to become airborne — intubations, for instance. In this room, air can circulate, but doesn’t leave the room. On the side is an anteroom where health-care workers “don” and “doff” their personal protective equipment in an ordered fashion. An ICU nurse called the “sheriff” watches to ensure it’s done correctly and to stop anyone who might run into the room.
All of those interviewed, given a chance to say what’s on their minds, thanked Islanders for the team effort, acknowledging that new cases of COVID-19 cases are falling and the health-care system remains robust because of everyone’s sacrifices. If they have a common request, it’s that as restrictions ease in the coming weeks and months, Islanders hold the line.
It’s hard to keep your cool even with safety protocols
Kelly Phillips, 28
• Critical-care registered nurse
• In job 5 years
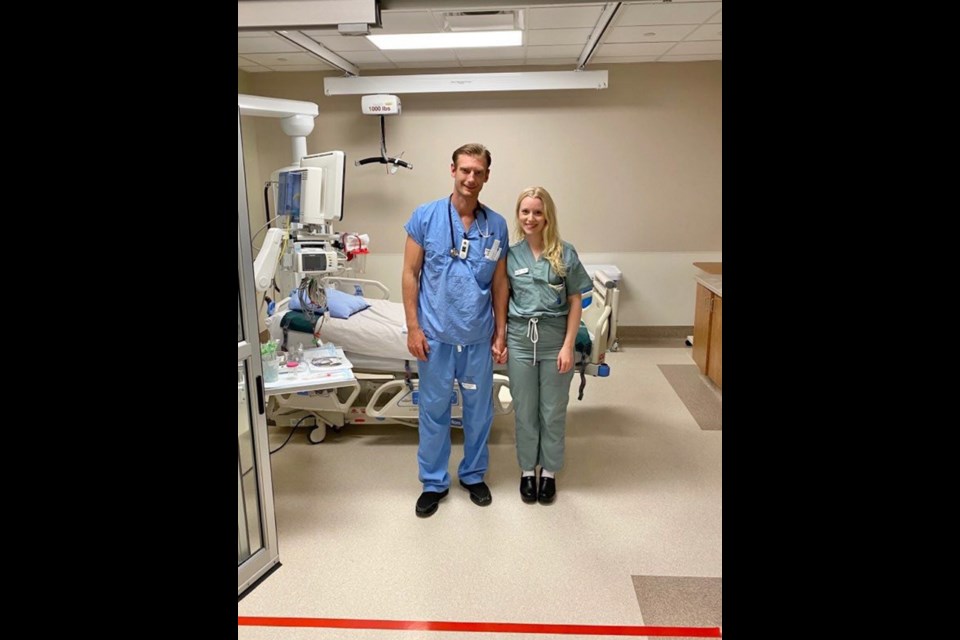
• Engaged to respiratory therapist Evan Janzen
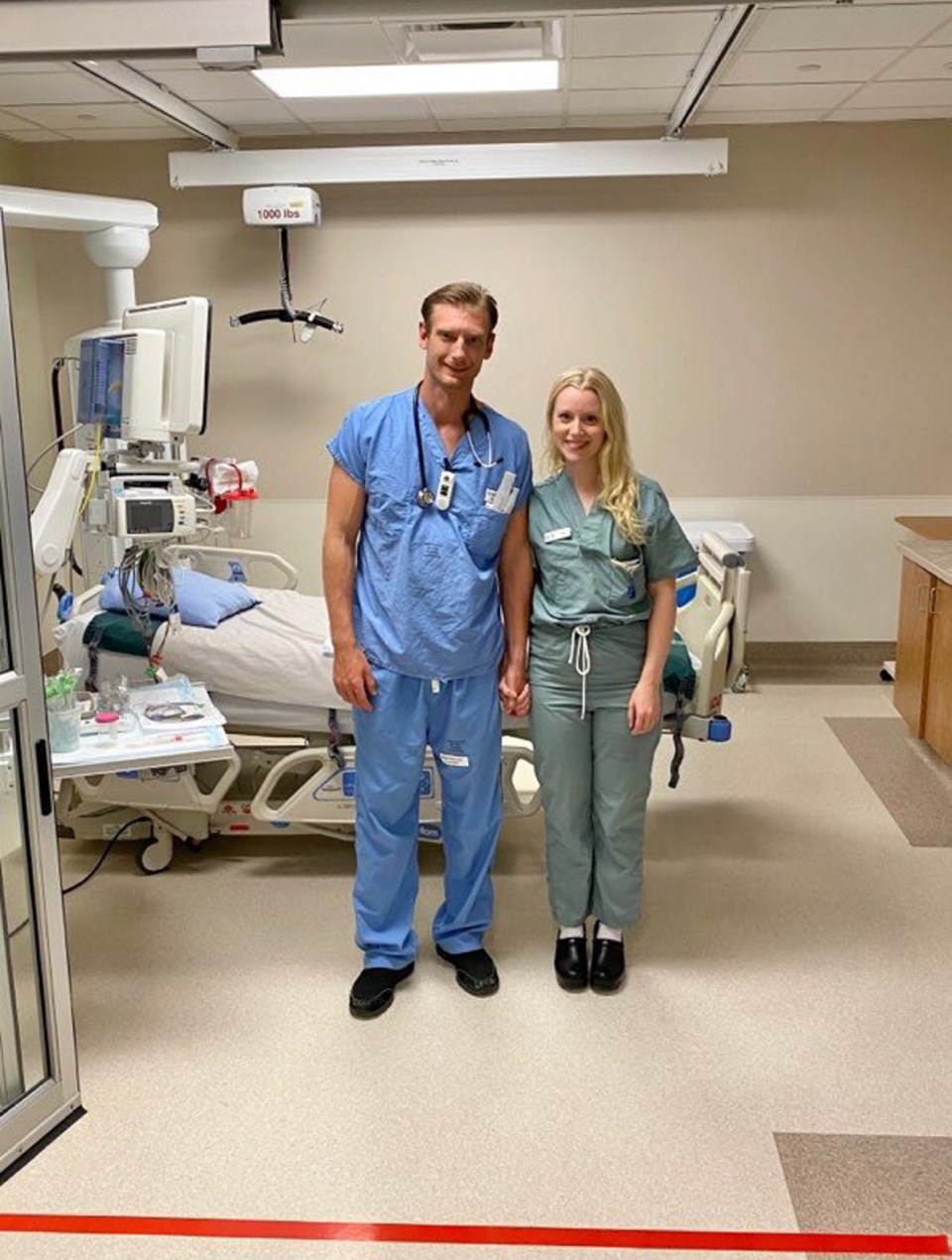
Kelly Phillips’ voice cracks with emotion as she talks about being at the bedside of a frightened young adult with COVID-19.
“Young healthy people, they’re really scared,” says the critical-care nurse. “Being able to be there to comfort them and get them through this illness has been a total privilege.”
“They have kids and they have a lot to lose, and so being with them and holding their hand while, you know, wearing all your personal protective equipment, is a pretty cool moment.”
Like her colleagues, Phillips struggles with the need to get to patients quickly, while putting on and taking off personal protective equipment in the right order to prevent contagion.
Because each ICU nurse is typically assigned one patient, she says, “we are very protective of our patient.”
“If alarms are going off, we are very quick to respond, and having that delay is emotionally taxing sometimes because you just want to get in there,” Phillips says. “There are many times you want to put yourself aside and you just want to go in that room and calm your patient and reassure them and stop that beep or change that bag or whatever you need to do, but you have to keep that in the back of your mind that you have to be safe.
“Our unit has adopted an attitude of ‘let’s slow things down, let’s not panic, we’re going to be safe, we’re going to be honest and we’re going to be very attentive to each other.’ ”
It’s not easy.
Even with all the safety protocols, unintentional exposure can happen.
Phillips cites a personal example: While she was moving a patient, a ventilator detached, causing “a massive amount of exposure.”
In those times, care providers become hyper-aware of their contacts and the incubation period for the virus — an infected person will typically develop symptoms within five days to 11 days, but it can be as long as 14 days before someone knows they are sick.
“It’s very stressful and you can feel responsible for everyone around you, as well as your own well-being,” she says.
Phillips considers herself lucky that her fiancé, respiratory therapist Evan Janzen, works in the same ICU and understands “the emotional roller-coaster” of working in a pandemic.
“We’ve both been in very close contact with multiple COVID patients, so we’re coming home together with the same amount of exposure.”
For now, they are isolating, and can’t visit Janzen’s sick father.
The couple’s summer wedding has also been postponed because of the pandemic.
“We joke about getting married in the ICU together,” Phillips says.
For paramedic, it’s a time of changing practices
Nic Hume, 37
• Paramedic based in Victoria
• In job 8 years
• Partner Anna Stefek, 30, paramedic

Every time paramedic Nic Hume puts on his mask and gets out of his ambulance, he has to assume that the patient he is helping is infected with COVID-19.
For every call, he has to wear a mask, a face shield and gloves, regardless of whether there are any COVID concerns, he says.
“There’s been so much change in the way we handle everything in the last few months,” Hume says. “Everything has slowed down and become very detail-oriented, especially around personal protective equipment.”
Each work day, Hume wakes before dawn and drives to Victoria from Sooke to start work by 6 a.m. For the next 12 hours, he doesn’t know when, or where he’ll go — just like in his former job as a newspaper photographer.
In the early days, it was stressful because there was so little known globally about the virus, he says.
The first suspected COVID-19 call was “unnerving.” Since then, he’s changed many practices. Work clothes stay at work and he receives a fresh uniform daily.
A self-described “nerd,” Hume says he was studying the disease early on, and by late February or early March, he had already said goodbye for now to his 96-year-old dad, columnist Jim Hume.
“There’s a very real chance I won’t see him until mid-summer, and at the age of 96, a lot can happen in those months. He’s in great shape. He still writes his blog every week … but.”
Nic Hume, who lives in Sooke with his partner, who is also a paramedic, says it’s never crossed their minds not to go into work because of the risk of infection.
“This is what we do. … This is a particularly unprecedented event in our lifetime, but this is what we signed up for.”
Having said that, the shifts under the shadow of COVID-19 seem longer and harder. Twelve hours in personal protective equipment — a mask, face shield and gloves — and the strict regimen of putting it on and taking it off is exhausting, he says.
“I feel significantly more tired now than I would have a few months ago, and I personally attribute that to being constantly vigilant about cross-contamination, being constantly vigilant about personal protective equipment.”
If there’s a bright side to the pandemic, it’s seeing people rise in the face of adversity and show kindness — food delivered to the front lines, drive-by cheers and drumming at the hospital, chalk art thanking all those in health care.
“It’s humbling.”
ER physician drills down for possible second wave
Dr. Matthew Carere, 36
• Emergency-room doctor
• Married, two children, ages 5 and 3
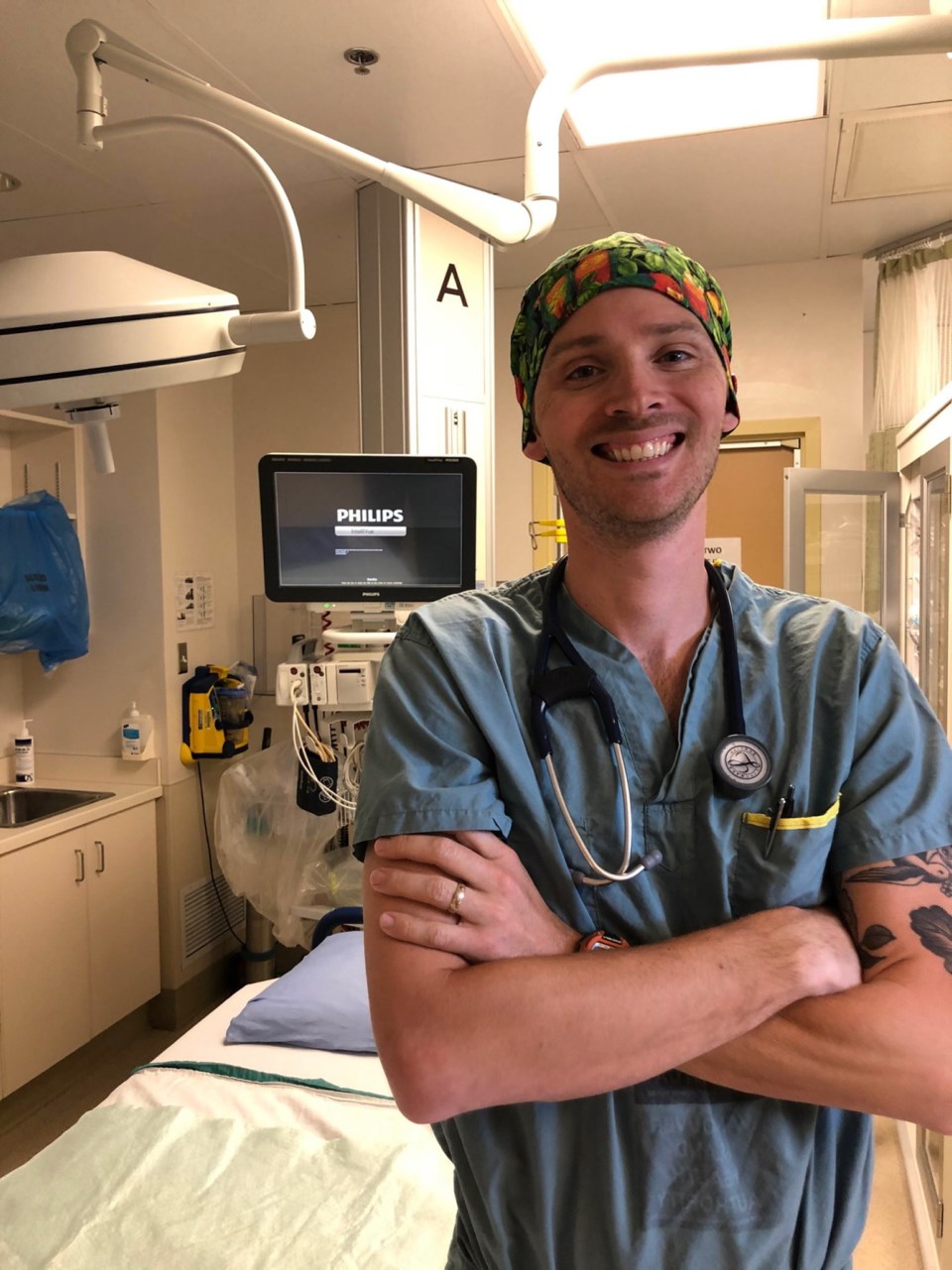
Emergency-room physician Matt Carere has been inspired by the rapid response to COVID-19 in Victoria, where simulations and preparations continue for a possible second wave.
At Royal Jubilee and Victoria General, he says, no stone has been left unturned.
“It’s crazy what’s happening here. Physical walls are being built on a daily basis. We’ve cordoned off areas. We’re inserting negative-pressure rooms. We’re changing the entire geography of hospitals, just to be ready for this.”
Carere says how rapidly the hospitals adapted made the pandemic feel real very quickly.
“When people are critically ill now and they’re coming into the emergency and if we don’t know their COVID status, we’re pretty much treating them as if they are likely to have COVID,” says Carere.
“It just adds one more layer, one more decision to an already very stressful situation.”
Previously, for example, an asthmatic child would be given medicine that would be humidified, but that procedure would aerosolize the virus, turning droplets into a far-reaching mist, “so we can’t ask a nurse to start that in the middle of the emergency room.”
Now, staff must don full personal protective equipment and put the child in a negative-pressure room. It’s the same for cardiac or kidney patients — the logistics are challenging.
Simulation drills could include an infant with breathing problems, a six-year-old with a seizure, patients with major traumas — all positive for COVID-19. “We’re preparing for all those eventualities.”
In the beginning, doctors were looking for coughs and fevers, then runny noses, headaches and muscle aches.
“Then it was vomiting and diarrhea,” Carere says. “You put those things together and basically anyone that comes into the emergency department has one of those things.”
Calming and connecting with ER patients is also tougher in a gown and mask. “Certainly with our pediatric patients, when they come in, you pull your mask down really quick and say: ‘this is my face’ to normalize the experience.
With reduced traffic in the emergency department as a result of the pandemic, he says, the level of care for sick patients is “quite excellent. Now we’re seeing heart attacks very fast. We see traumas right away.”
Carere says people who work in critical and emergent care tend to be risk-tolerant, but COVID-19 has caused everyone to change their ways. Many physicians shower at work so as not to bring contaminants home. “One doctor installed a shower outside of his house.”
Carere says he’s indebted to Vancouver Islanders for staying home and decreasing the patient volume.
“We have a low caseload on the Island, but if we had the pre-COVID volume in our hospital going on while we were trying to change everything and get ready, it just wouldn’t be possible. We wouldn’t be ready.”
Personal protective gear a blessing and a curse
Shannon McGregor-Brown, 43
• Critical-care registered nurse
• In job 11 years
• Married with a five-year-old son

The personal protective equipment that every critical-care nurse depends on for safety is one of the most frustrating aspects of dealing with the pandemic, says Shannon McGregor-Brown.
“I think that’s probably the most stressful part, sometimes, is not being able to get to your patient in the time that you want to solve the problem that you know you can solve.”
Care providers can track their patients’ vital signs from a central monitor at the main desk in the intensive care unit and via patients’ bedside monitors that can be seen through glass walls and doors. They can see whether blood pressure is dropping, or if sedation medication is running low or ventilator requirements change.
But before they can get to a patient, they have to stop and put on protective equipment.
It’s both a blessing and a curse to those in emergency and critical care, especially with COVID-19 patients, because of how rapidly they get sick, said McGregor-Brown. “They come in and we intubate them if their oxygen requirements are tipping and then we ventilate them, and sometimes it just cascades so quickly.”
They might need a renal-dialysis machine to filter their blood of toxins. Antibodies can cause an inflammatory response and there is a possibility of blood clots. There can also be cardiac issues.
“So there’s all these physiological changes that can happen over a period of time — sometimes it’s a few hours and sometimes it’s over the course of days — and some days you think they’re getting better and then they take another turn.
“Suddenly their pressure is dropping and … you’re trying to maybe run dialysis and make sure that their kidneys are going to pull through in the end of this … You can’t keep their blood pressure up — it’s a cascade of events.”
Not knowing how this virus is going to respond in any one person’s body is the thing that keeps her up at night.
“It’s a crapshoot,” she says.
In March, McGregor-Brown had to call a family in Saskatchewan and suggest they drive out to see a patient immediately. “This person was declining rapidly and it broke my heart. They’re saying to me: ‘I don’t know when I come there, am
I coming to see my brother alive and to say hello, or am I coming there to collect his body and take him away?”
McGregor-Brown didn’t know, either. “We take things literally hour by hour, if not minute by minute, when they’re critically ill here, and you just try to support that family to the utmost.”
McGregor-Brown’s husband, Michael Brown, who works in finance, is working at home during the quarantine. She considered self-isolating, but couldn’t bear two or more months away from her five-year-old son. She exercises extreme caution about hygiene.
She likens COVID-19 to a monster in a dark room. “[At first] we hadn’t turned the lights on yet to see what the monster is, but now that we’ve seen it and worked with it, I feel more confident when I go home.”
From feeling strange to feeling appreciated
Toni Barkanyi, 40
• Royal Jubilee housekeeper for 9 years
• Married, two daughters, ages 22 and 17
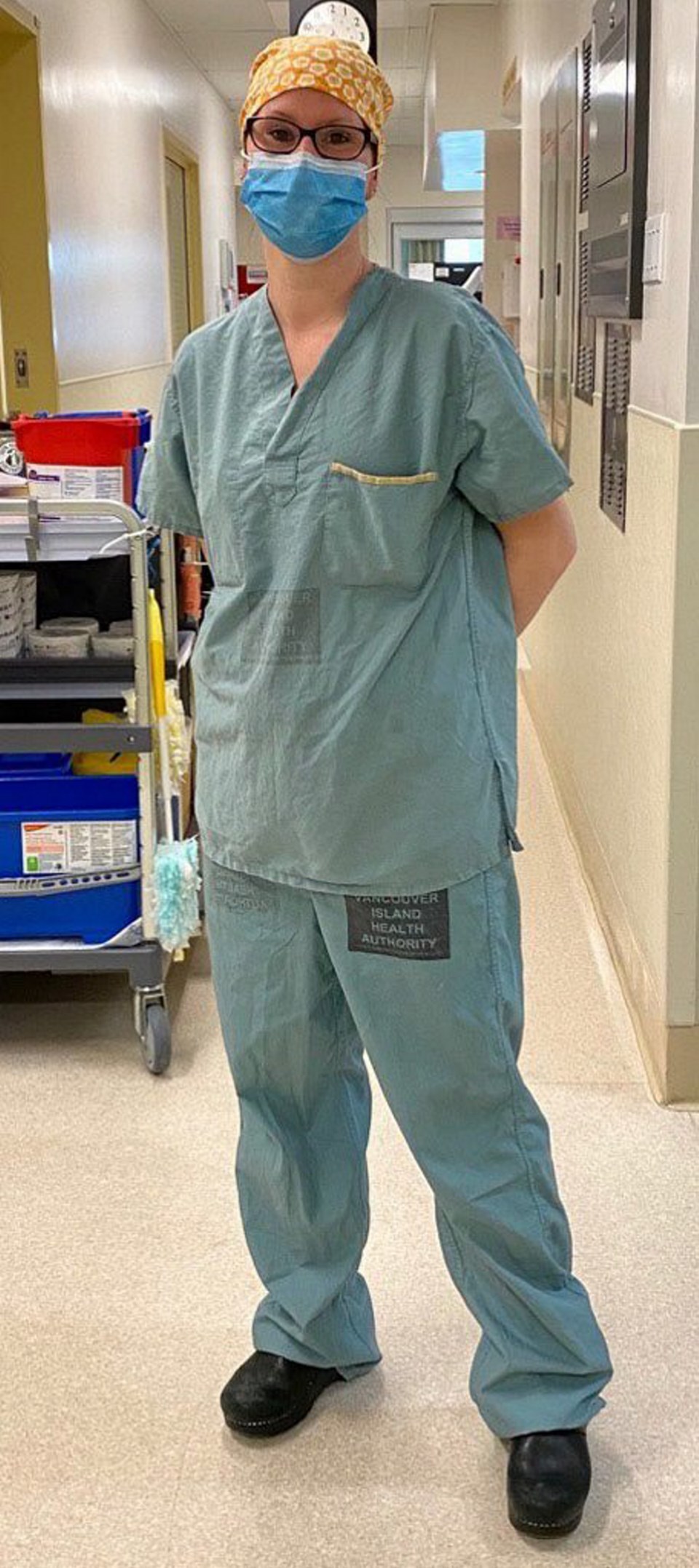
After the intubation of a COVID-19 patient — where a tube is inserted through the mouth into the airway, sending aerosolized particles into the negative-pressure room — the specialists leave and housekeeper Toni Barkanyi moves in to wipe the room clean and remove the hazardous waste.
In the intensive care unit, she’s responsible for cleaning the entire area, including patient rooms — washing the linens, removing the garbage, mopping the floors and wiping down all “touch” areas.
“I have to make sure the space is safe,” she said.
In the early days of the pandemic, when she hadn’t yet received instruction from her union on protocols, she followed nurses and doctors in the ICU, listening in on their huddles on how to stay safe. She made sure a nurse watched her don and doff her personal protective equipment, both for her sake and that of patients.
Barkanyi worried about bringing the virus home to her husband and children, but felt a responsibility to do her job as part of a team.
“I felt that they are also my patients,” Barkanyi says. “I clean like I’m cleaning for my family. I can’t think of any other way to do it.”
On the hardest days, she had multiple daily cleans on multiple COVID-19 rooms.
“It’s a long process and it is quite draining, putting on and taking off your personal protective equipment and making sure everything is right, perfect. And then going into the next room and the same routine.”
It took weeks for her to become accustomed to the new protocols and confident that she could keep herself and others safe.
In the early weeks, Barkanyi thought the 7 p.m. cheers for health-care workers had nothing to do with her.
“It was a little strange for me, because I thought this is just for doctors and nurses, you know. Then eventually, over the course of that time, I started hearing more about the behind-the-scenes workers, housekeeping, the instrument cleaners, everybody else. And then
I started feeling really appreciated.”
In a COVID-19 patient’s room, there may only be a doctor, respiratory therapist and a nurse, but before and afterwards, there’s a cleaner.
“I’m proud to be a part of that.”
Supportive team helps her cope with pressure
Shaelyn Allen, 29
• Critical-care registered nurse
• In job five years
• Married
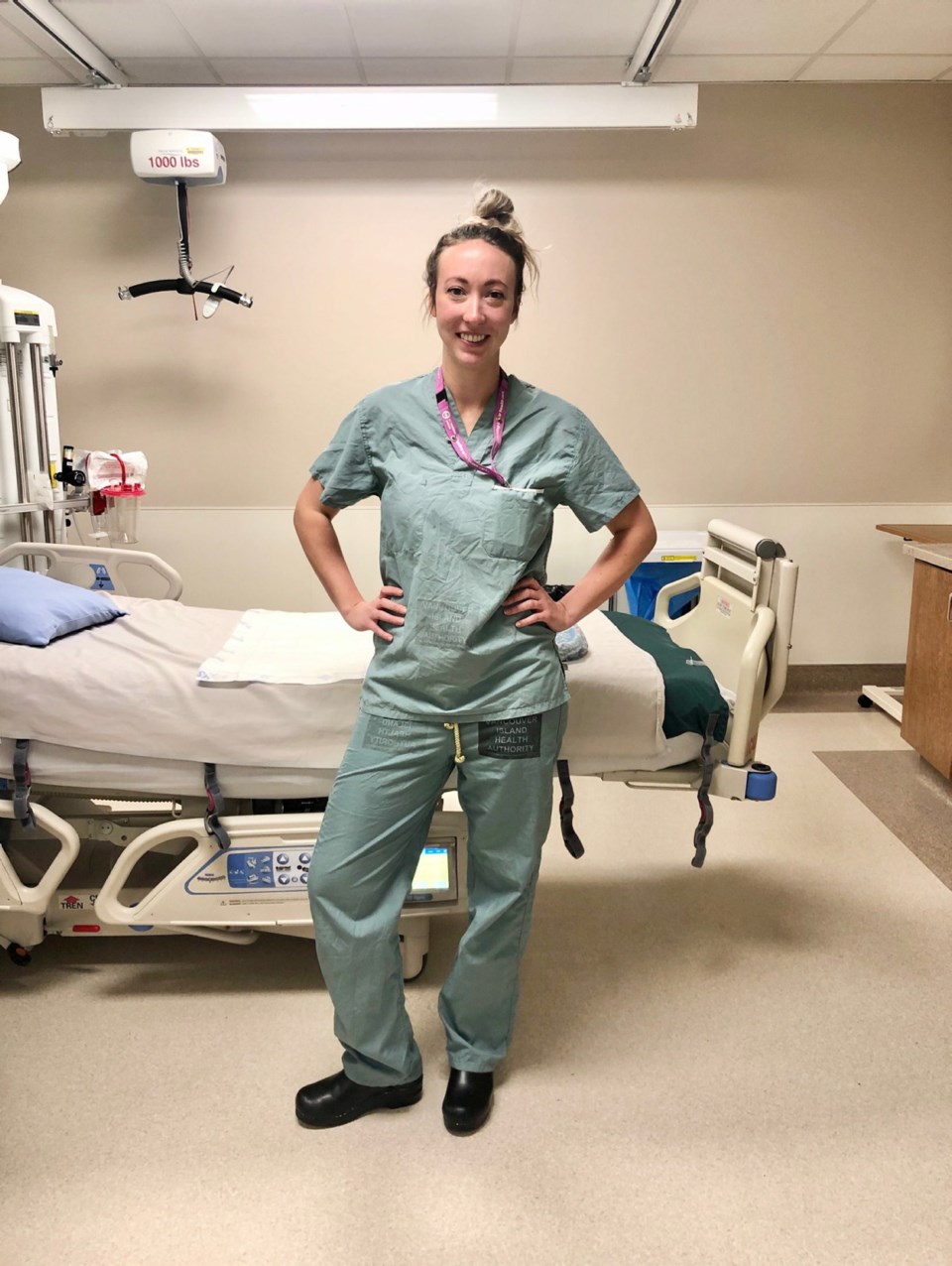
Shaelyn Allen says trying to keep COVID-19 patients and their families connected is tough.
“The hardest thing for me is having the families not be able to come in and visit their loved ones when they are so sick,” Allen says. “With nursing, it’s a holistic approach. We don’t just nurse the patient — we nurse the family as well.”
Allen says her own family — along with colleagues and a phenomenal interdisciplinary team and great leadership — helps her get through when the anxiety of the COVID-19 crisis mounts.
“Knowing you work with such an incredible supportive team has really helped.”
While being quick-thinking and fast-acting in a medical emergency is the “bread and butter” of those working in the ICU, Allen says slow and methodical is key in the pandemic.
“Your first instinct is to run into the room when something’s wrong. But now we have to step back and we have to make sure we’re protecting ourselves and we’re doing the right things in the right order,” she says, noting different personal protective equipment is required for different procedures.
“So knowing instantly which PPE to put on and getting into the room to do your job is quite stressful, to be honest, and it’s been a bit of a challenge and a learning curve, but I feel like we’ve learned pretty quick on the job as to what needs to be done and making sure we’re protecting ourselves.”
Allen was hoping to start a family this year, but she and her husband have put that on hold for now, “just for safety.”
Much is still unknown about COVID-19, says Allen, which can lead to a feeling of helplessness and lack of control. “You don’t really know what you’re going into … when you enter the patient’s room.”
A patient who seems to be recovering can “turn, like almost instantly,” she says, adding she’s only had one “bad breakdown,” after her first COVID-19 patient.
“It was just the pressure,” she says. “This is like something completely new — you don’t exactly know what you’re looking for. You don’t exactly know what to expect. The treatment is different, too, and because there’s no cure and there’s no straight-up treatment, you’re just kind of doing symptom management.”
On tough days, she says, she powers through remembering who she is doing it all for: her patients and the community.
“We hear that they’re cheering for us all the time. We really appreciate the support of the community. We couldn’t do it without them.”
Boxes of gear in her office protect patients and staff
Carrie Homuth, 49
• Manager, adult intensive care units, 23 years
• Royal Jubilee Hospital and Victoria General Hospital
• Married with two grown children

Carrie Homuth shares her office with boxes of personal protective equipment.
In the early days of the pandemic, she was tasked with planning for the intensive-care units of Vancouver Island’s two main hospitals, which felt like being at war, she says.
If she was to protect patients, she had to first protect staff. At first, it was not clear how much gear they had or how much they could attain in a global pandemic. “My office got turned into a warehouse,” says Homuth. Back-up equipment was stockpiled and kept under lock and key.
With the boxes under her nose, her department knew exactly how much they had for how many staff, patients and procedures. “That gave us a sense of control and took away a lot of fear,” she says.
Planning went into overdrive in March. How would the hospitals treat 100 patients requiring intensive-care services? How would they get enough personal protective equipment?
“The pressure was on us to prepare as much as we could,” Homuth says.
Rallying the troops meant being able to ensure they would be safe coming to work. Staff were being asked to potentially care for hundreds or even thousands of sick and dying.
“It was stressful,” Homuth says. “At that time, it seemed like every day was a gift to get a little more preparation done and now it’s a gift that the worst hasn’t happened.”
As the daily number of new COVID-19 cases on Vancouver Island wanes, Homuth says officials are continuing to plan for a potential second wave in the late fall, combined with influenza season.
“It’s a constant tension between planning for what is unimaginable and dealing with what’s in front of you,” says Homuth, who had taken only five days off over seven weeks.
“Sleep isn’t really happening anymore. I think as much as you step away from work physically, emotionally and mentally, it still plays in your mind 24/7.”
Homuth says she’s either in her office, car or house, oblivious of the outside world.
The pandemic has forced the postponement of her son’s wedding, planned for Merridale cidery this summer.
“That’s a little sad.”
Worried about patients, and spreading the virus
Leigh Walters, 51
• Respiratory therapist
• Royal Jubilee Hospital
• On the job 18 years
• Married, two sons 12, 14

When a Code Blue is called over a hospital intercom, “things are really bad,” says respiratory therapist Leigh Walters.
It’s typically an impending cardiac or respiratory arrest. In her younger days, she would have felt an adrenaline rush. It’s different now: “At this point in my life, I always think: That’s awful.”
Walters has enough experience intubating and extubating patients, giving CPR and assessing people unable to breathe that she doesn’t need that adrenaline to power through.
Those first few weeks intubating COVID-19 patients were “incredibly stressful,” she says, as no one knew enough about the disease. After performing an intubation, she’d worry about spreading the virus.
“I was anxious. That anxiety and those early days of doing those intubations was something that I found very challenging.”
She didn’t realize the toll it was taking until she found herself waking at 3 a.m. after bad dreams.
Although she took every precaution not to bring the virus home, she soon made the decision with her wife and her two children to self-isolate. “My kids are young and my wife, I was concerned about her.”
One of the things that sets COVID-19 apart is how quickly a patient can deteriorate, she says. “We need to act really quickly, in a very controlled manner.
“We’re shutting things down, we’re putting on negative pressure, we’re all getting into our gear and we’re doing things with a very specific process that’s developed to ensure that we are safe, that our patients are safe, and that the rest of the emergency department is safe.
It’s hard, she says: As with other health-care workers, her impulse is “just to go. That’s the nature of respiratory therapy. We just go and we do.”
Walters says she is grateful to live on an island where people have taken the measures needed to keep infection rates low. And she’s a fan of the woman at the helm in this pandemic: “Dr. Henry … she is my source of truth.”
The threat of a surge or another, bigger wave rarely leaves her mind.
Her worst fear is that a work colleague will become infected. But she says no one will walk away unaffected by the pandemic.
“I think for all health-care workers, this will leave a little bit of a mark.”
- - -
To comment on this article, send a letter to the editor.
• Email: [email protected]
• Mail: Letters to the editor, Times Colonist, 2621 Douglas St., Victoria, B.C. V8T 4M2.
Letters should be no longer than 250 words and may be edited for length, legality or clarity. Avoid emailing your letter as an attachment. Please include contact information; we require your first and last name and the municipality where you live for the letter to be considered for publication.