This story is part of an ongoing look at the challenges facing the health-care system in Greater Victoria and B.C. Future stories will look at possible solutions, things that are working well, and the B.C. government’s ongoing efforts to reform primary health care.
Until recently, Barbara Pedrick never had to worry about finding a doctor. For nearly 40 years, she saw the same family physician in James Bay. He helped her through cancer treatment and recovery, performed regular checkups and kept track of her lab tests and medical records.
“He delayed retiring for I don’t know how many years, because he couldn’t find somebody to replace him,” Pedrick said.
Eventually, though, he had to quit, and Pedrick has been unable to find a permanent replacement.
“I’ve called a few places,” she said. “I couldn’t get anyone.”
Instead, like thousands of people in Greater Victoria and across B.C., she now relies on walk-in clinics, which she says are a poor substitute for the continuum of care she once received from her family doctor.
By way of example, she cited her last visit to a clinic to get a referral for a diagnostic mammogram — something she’s expected to do regularly as a breast-cancer survivor. The people at the clinic were very pleasant, she said, and obtaining the referral was no problem.
But they showed no interest in seeing her medical records, and when she inquired about getting an annual physical examination, a doctor told her the clinic no longer performed them.

“I said: ‘Well how do we keep track of things and how do I get the blood work that you get done at an annual checkup?’ He said: ‘Well, you can come in and ask me, and I’ll order any blood work that you want.’
“I’m sure you can hear the problem with that,” Pedrick said. “How do I know? I don’t read The Lancet. I don’t keep up with medical progress.
“The point of an annual physical exam is that your doctor will have new information because hard-working doctors keep up with the newest information. So you go in for your annual physical and the doctor may know: ‘Oh, a new thing has just come up. Let’s check this for you.’ I don’t know that.”
The experience, she said, left her shaken and angry about the sorry state of primary health care in B.C. as it exists today.
“We need more family doctors,” she said. “It is my opinion, and the opinion of a lot of other people, that a good family doctor, who knows you, who is aware of your health history, and who oversees and manages your care, is the best preventative medicine there is.
“Clinics are fine in an emergency,” she added, “but as my experience shows you, they will not offer me that kind of care and oversight and attention that really creates a good health-care program.”
- - -
Tell us your story
Have you been affected by this issue, or do you have an idea for a story? We’d love to hear from you.
Send an email to [email protected] with the word “doctors” in the subject line, send us a tweet at @timescolonist using the hashtag #TCdoctors or join the conversation on our Facebook page. We’ll share some of your stories as part of our series.
- - -
Pedrick is far from alone in that assessment. Physicians, researchers and other patients say the difficulties getting access to a family doctor in the capital region and in other parts of the province are stretching primary care to the breaking point.
Each morning, people line up outside clinics across the capital region to make sure they get an appointment for that day.
In Sidney, a line of senior citizens can be seen snaking down the block an hour before the Shoreline Medical clinic opens.
“It looks like a movie theatre out there, people bring their chairs,” Dr. Gordon Henderson said. “The doors open at 8:30 a.m., but I often come in at 7:30 a.m. to do paperwork and people are there, in line.”
The 60-year-old physician called it “outrageous” that so many seniors have no family doctor.
“It’s gone beyond a doctor shortage — it’s a crisis,” he said. “Ninety-plus-year-olds without a family doctor, that’s not OK.”
Statistics Canada says 97,800 people — or nearly 15 per cent of the population age 12 and older on Vancouver Island — had no regular health-care provider in 2015-2016, the most recent period for which statistics were available.
The problem was even more pronounced in the capital region, where 18 per cent of the population or nearly 60,000 people had no regular provider, a category that includes family doctors, medical specialists and nurse practitioners.
The problem persists, despite the fact Canada actually has more doctors — and more doctors per capita — than ever before, according to statistics from the Canadian Institute for Health Information.
So what’s going on? If there are so many doctors, why can’t people such as Pedrick find one to care for them?
Physicians and researchers say there’s no simple answer to that question, that there is a “perfect storm” of factors at work. For one thing, many doctors are seeing fewer patients, in part because they want a better work-life balance than their predecessors, but also because the cases they handle are becoming increasingly complex as the population ages.
At the same time, doctors young and old are rejecting the traditional family practice for reasons ranging from the complex fee-for-service payment system to the administrative burden of running a business.
Dr. Eric Cadesky, past president of Doctors of B.C., says the “shortage” is less about absolute numbers than a failure to use the doctors we have more efficiently by supporting them with teams of other professionals who can share the workload.
“What could have been done by one doctor years ago may take two or three or more doctors to be able to keep up that same level of work today, because the demands have increased exponentially,” he said.
Dr. Michael Rachlis, health policy analyst and adjunct professor at the University of Toronto’s Dalla Lana School of Public Health, says that, unfortunately, there’s still very little primary-care teamwork, despite widespread recognition that it’s critical for effective health care.
“We’ve gone from maybe Es to D-minuses in Canada in primary healthcare teamwork,” he said. “We could be doing so much better.
“And if family physicians didn’t have to see 50 per cent of the people they see every day or more, then they would have lots of time for you and me when we are really sick and we need somebody who has the unique skills and diagnoses and therapeutics that doctors have.”
B.C. Health Minister Adrian Dix has embraced the team-based approach as part of a three-pronged strategy to open urgent primary care centres, develop primary care networks and expand community health centres.
“I think we are engaging in the most significant reform of primary care that’s occurred since the start of Medicare,” he said in an interview.
But major health-care reforms don’t happen overnight. In the meantime, family physicans say their colleagues are experiencing high rates of burnout because of the increasingly complex cases they face, a time-consuming electronic records system, the administrative burden of running an office, and a fee-for-service system that rewards high-volume practices, penalizes doctors who spend additional time with a patient and neglects to compensate physicians for all the paperwork they have to complete.
As a result, family physician Dr. Jennifer Lush, 44, says primary care is on the brink of collapse in Greater Victoria.
“I’ve never seen it like this,” she said. “It’s truly a dire situation here.”
Lush, who was born in Victoria, earned her medical degree in B.C. and has practised as a family doctor here since 2002. She took over a practice of about 1,500 patients from a retiring physician in 2016 and regularly sits up most nights to catch up on her chart notes and lab results, arrange referrals and send emails — sometimes until 1 or 2 a.m.
Maintaining patient charts is crucial for a patients’ long-term care and best outcomes, but Lush said she feels like a “hamster on a wheel racing to keep up.”
“I think most family physicians love primary care and went into it with the best of intentions but, unfortunately, we are losing so many of them because the problems are so endemic and pervasive even the most well-intentioned doctors are reaching their breaking point,” she said.
Most family doctors are paid a so-called fee for service — payments provided for each service provided. However, doctors generally say the compensation is not enough and the billing system is complex and time consuming.
Lush noted that she gets paid the same if she sees a patient for five minutes or 45 minutes — “which happens not infrequently because one medical issues becomes a counseling visit and then they mention a chest pain and I have to work that up.”
Dr. Bridget Reidy, who took over a family practice from a retiring physician in Saanichton more than two years ago, sees mainly geriatric and complex-care patients. She says the fee-for-service model used in B.C. doesn’t compensate physicians fairly for treating this patient group, which requires additional time.
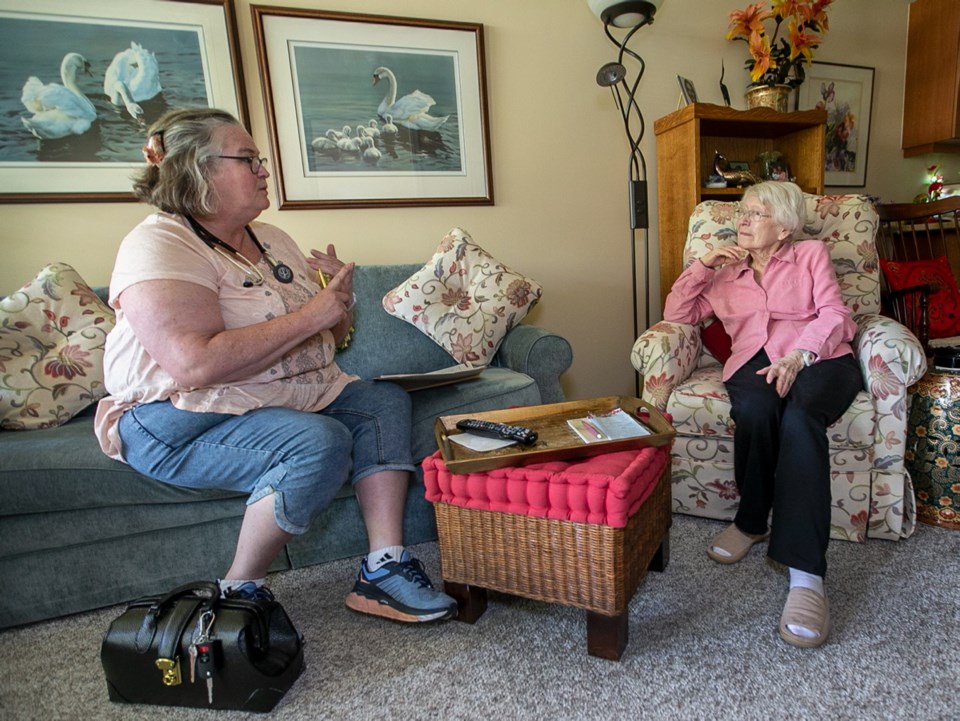
To get by, Reidy works at the Royal Oak Medical Clinic one day a week to earn extra money.
“I go to the walk-in clinic to support my chronic-care habit,” she said. “I don’t think I would have made it without the walk-in.”
Faced with such pressures, many doctors are walking away and choosing to take salaried jobs as hospitalists where they make good money, work in a team environment, and pay none of the high overhead costs that family doctors do, said Dr. Vanessa Young, chairwoman of the South Island Division of Family Practice.
“There is no shortage of GPs,” she said. “There is a shortage in the community, providing comprehensive continual and compassionate care, amid a dying business model.”
Further compounding the problem, new doctors are steering clear of family practice for the same reasons that so many veteran doctors are leaving.
Dr. Rita McCracken, a family physician and researcher at the University of B.C., said 40-50 per cent of medical students are choosing family practice for residency, but only 15 per cent of those who finish the residency choose to work in the traditional family practice model.
“We’ve known this since at least 2012 when the first paper was published based on British Columbia data, saying that new graduates don’t want to work this way. In truth, it’s been known for longer than that.”
Governments, however, have been slow to reform the fee-for-service model that doctors, both new and old, reject as cumbersome, unfair and outdated, McCracken said.
“As a result, the problem’s just getting worse and the problem’s going to keep getting worse.”
In the absence of immediate reform, McCracken said medical school graduates are remaking the system themselves, and she said they want the same things as everybody else.
“They want a job that they can count on, that is going to have a reliable source of income, where a good portion of your day doesn’t have to be [spent] tracking down and enumerating every single element that you have done. They want to be supported. They want to work in a team. They want to be able to take a vacation or have a baby,” she said.
“They’re not looking for hundreds of thousands of dollars more a year; they’re looking for a job environment that most Canadians also aspire to.”
Instead of opening a family practice and providing continuing care to patients in the community, they might work a couple of shifts as a hospitalist, two or three half-days in a health authority owned-and-operated care clinic and few shifts at a walk-in clinic, McCracken said.
“The really amazing thing is that we see new graduates in British Columbia have, on average, 2.6 locations that they are working in,” she said. “So they are doing a whole bunch of things to create a job environment that is more attractive to them. We have not changed the structure in which they can work, so they have changed the structure.”
The downside, experts say, is that patients have fewer places to go for the type of comprehensive, continuing care that they traditionally received from a trusted family doctor with whom they developed a long-term relationship.
Instead, they’re often receiving episodic and potentially more expensive care at walk-in clinics or hospital emergency departments.
Physicians say there are a number of fundamental risks with such a fragmented system.
“One is that important symptoms can get lost,” McCracken said.
She pointed to a case in Nova Scotia where a young mother posted a video on Facebook in April, describing how her cancer went undiagnosed for two years because she had no family doctor and was repeatedly turned away by emergency departments.
“That’s a most tragic example of what happens when you’re seeing a new provider each time and where your whole person is not able to be considered,” McCracken said. “That’s the magic sauce of primary care — that relationship with a team and individuals who get to know you as a person [and] where you’re not needing to tell your whole story over and over again.”
The other problem, McCracken says, is that care will become more costly and invasive if people are forced to rely on walk-in clinics and emergency room medicine.

“If we’re only seeing one person at one time, we might order excessive numbers of investigations and tests in an effort to try to know the thing that we can’t know without the relationship,” she said.
There are other downsides. Dr. Peter Gladstone, a cardiologist, sees thousands of patients each year for heart attacks, valve heart disease and cardiac surgery.
“Probably somewhere in the range of 25 per cent of those have no primary care physician, which means they are out in the community, basically orphaned,” he said.
Gladstone says primary care is the bedrock of the health-care system and, without ongoing monitoring by a family physician, cardiac patents have a higher mortality rate no matter what miraculous surgery is done in the hospital.
“What happens is we see them coming back for preventable things, aside from the anxiety issues of being left to spin in the wind,” he said. “They go back to the emergency department or walk-in clinics, which bandage the problem.”
Dr. Greg Rideout says primary care has “collapsed” in the region. A family physician who moved to Victoria from St. John’s in late 2016, Rideout said he was astounded by the number of walk-in clinics in Victoria, the cost of living and the overhead required to operate a family practice.
Rideout said he did good work in walk-in clinics but grew concerned about the number of complex-care patients who might be diabetic with a heart condition, for instance, getting multiple duplicate tests because they were bouncing out of necessity or convenience from one walk-in clinic to the next.
“That became a stressor and that’s kind of what forced me back to my own clinic.” He bought into Oak Bay Medical Clinic as a full-time family physician in September 2018.
“There’s no shortage of patients,” Rideout said. “We were totally overwhelmed and bombarded with people who legitimately all needed care. There were a lot of complex care patients who weren’t getting regular care.”
Rideout said he’s working harder and making less money than he was in St. John’s 15 years ago. He calls the billing system almost “frightening and undo-able,” and says he works after dinner each night to complete necessary paperwork.
“I left work last night at 11 p.m. doing chart work,” Rideout said.
“My sense of primary care here is it needs radical change.”
Until that happens, people will continue having problems finding a family doctor, experts say.
Dr. Robert Brown, a family physician and medical director of the Ocean Pier Medical Centre in Sidney, said his office, which has eight physicians and two registered nurses, advertises constantly to attract new doctors. “We just don’t get anybody.”
As a result, Brown, 69, continues to work a slightly reduced work week.
“I feel like I can’t really quit,” he said. “I can’t find anybody else to take over my practice. But the patients that you know with complicated medical problems, you don’t just want to turn them loose.”
It’s a major worry for him and others, he said. “Us older guys, well, we’re sort of thinking, ‘What are we going to do?’ We don’t have anybody to pass the baton to.”
— With a file from The Canadian Press



