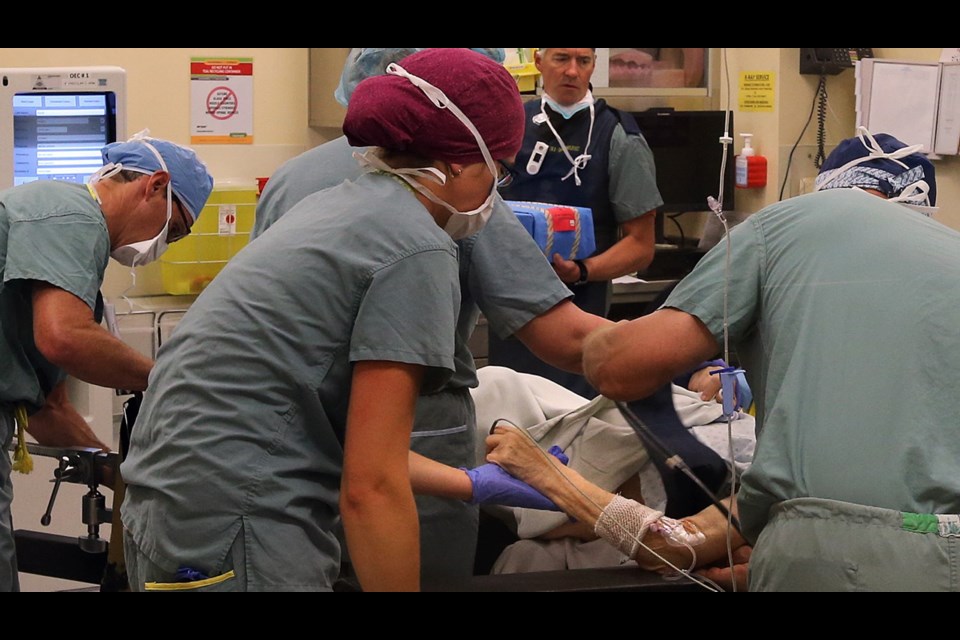
A dramatic increase in the number of hip-fracture surgeries done within 48 hours at Royal Jubilee Hospital is decreasing complications, saving money and maybe saving lives.
Weekend operating time for hip surgeries has been blocked off and interventions have been made as part of a provincial hip-fracture redesign project pilot program implemented at eight sites across B.C., including Royal Jubilee Hospital in Victoria.
Over the last three months, the overall number of patients showing up at Royal Jubilee’s emergency department with a hip fracture and operated on within the provincial benchmark of 48 hours has jumped — to 95 per cent from 74 per cent.
On the weekends, patients had a 49 per cent chance of waiting more than 48 hours for surgery. Now it’s five per cent, and instead of provincial benchmarks being broken, they are being exceeded.
The pilot program’s leader in Victoria, orthopedic surgeon Dr. Patrick McAllister, said that in the past, if a patient came to hospital late Thursday, Friday or Saturday, they would too often have to wait for surgery.
“That’s because hip fractures were competing with everybody else on the weekend — from the aneurysms, to the broken ankles, to the open heart surgeries, to the bowels and all that,” McAllister said.
Each year in B.C., almost 4,000 people fall and break a hip, according to the B.C. Ministry of Health.
It’s an injury that can turn an independent senior into a dependent senior.
The number of hip fractures is increasing at a rate of about two per cent a year. With an aging population, that statistic shows no sign of slowing without intervention and prevention programs. The average age of a person who suffers hip fracture is 81.
In March 2013, the B.C. Ministry of Health and Doctors of B.C. (formerly the B.C. Medical Association) announced funding for 21 programs initiated by doctors to support innovation in the health system.
The projects were chosen by the joint Specialist Services Committee, a group of doctors and health ministry staff.
The committee provided start-up costs of $799,000 from the already established Physician Master Agreement. Already, Island Heath has started to implement the program in Nanaimo Regional General Hospital and plans to expand it to other hospitals.
The B.C. pilot program has four phases (the first three of which have been completed): Gathering baseline data on hip-fracture care from 28 hospital sites in B.C.; using a secure web-based system to build a B.C. hip-fracture registry to serve all hospital sites; implementing best practices before and after surgery and innovation at eight pilot sites; measuring the results during two time periods; creating a report, plan and costs for implementation across B.C.
The use of hospitalists — who are in a heated labour dispute with Island Health in Victoria, which has the potential to put the program at risk here — and a 2011 National Hip Fracture Model of Care tool kit, which includes guidelines for the best practice of care with input from B.C. experts is also integral to the program’s success.
But perhaps the single biggest contributor to improving the current wait times at Royal Jubilee Hospital was Island Health’s decision, after considering the data presented by physicians, to dedicate a three-hour block of already available operating room time on Sundays, solely to hip-fracture surgery.
Two operating rooms are open on Sunday and there are always two orthopedic surgeons on call in Victoria and available on the weekends, but they couldn’t get into the operating room in a timely manner.
Too often, said McAllister, the frail elderly were not considered a priority in the health-care system. Their hip fractures lost out to surgeons who needed operating room time for more dire problems, he said.
“It’s hard for me to go to a vascular surgeon and say my broken hip is more urgent than your carotid artery or dead gallbladder,” McAllister said.
It was that understandable competition in the context of restricted access to operating room time that was causing serious post-surgery complications and increased rates of mortality for mostly older and sicker patients with broken hips.
“We are lucky in Victoria in that we have access to the operating room for fracture time Monday through Friday,” said McAllister. “But we knew our problem was … through the weekend.” People breaking a hip on a Friday sometimes weren’t getting surgery until Monday or Tuesday.
“We targeted hip fractures because they are the patients that have the highest impact on morbidity and mortality,” McAllister said.
The longer an older, frail and immobile patient with perhaps several health problems lies in bed, the greater their chance of what some might call supine crucifixion — pressure sores, pneumonia, blood clots, delirium, urinary tract infections and side-effects from pain medication.
“The older you are and the sicker you are, the longer you wait, the bigger the problem,” McAllister said.
Rates of post-operative complications such as urinary tract infections, side-effects from pain medication and cardiac occurrences are also down since the pilot project began in all heath authorities across the province, according to the Health Ministry.
Other pilot changes include a post-surgical team — made up of several disciplines and including hospitalists — becoming involved with the patient earlier in the hope of avoiding the increased risks of complications that come with the frail elderly.
“I’m a big-picture kind of guy, so as a surgeon it’s nice to get surgery done and not have patients waiting around, but there’s a lot more we can do and should be doing to make the system better,” McAllister said. “But within the system, it’s a bit frustrating to try to tie all the bits and pieces together because, as you know, with health-care budgets there are multiple draws for the same dollar and pressing and competing priorities.”
Island Health’s program funding ends in November 2015. The health authority has applied for an extension. The funding ends for the other pilots in 2015.
The provincial co-leads for the program are Dr. Pierre Guy, an associate professor and clinician scientist in the orthopedics department of the University of B.C. and Dr. Kenneth Hughes, an orthopedic surgeon based in Richmond and former president of the B.C. Orthopedic Association.
In data they collected and published with several other contributors under the B.C. Hip Fracture Redesign, they note that after breaking a hip, 30 per cent of patients die in the first year and 50 per cent lose mobility. McAllister adds that five per cent will die in hospital and there’s a 25 per cent chance that at some point the patient will break the other hip.
The pilot program is also running at Lions Gate Hospital in North Vancouver; Richmond General Hospital; Vancouver General Hospital; St. Paul’s Hospital in Vancouver; Burnaby General Hospital; Kelowna General Hospital; and University Hospital of Northern British Columbia in Prince George.
The pilot program here is similar to programs established in the U.K. and Sweden.
“In recent years, Sweden and the United Kingdom have both put in co-ordinated, evidence-based initiatives that include hip-fracture registries, performance measurements and implementation of best practices, achieving 15 per cent reduction in mortality and five per cent reduction in bed days,” according to the Health Ministry.
More on the hip fracture redesign can be found through: www.sscbc.ca