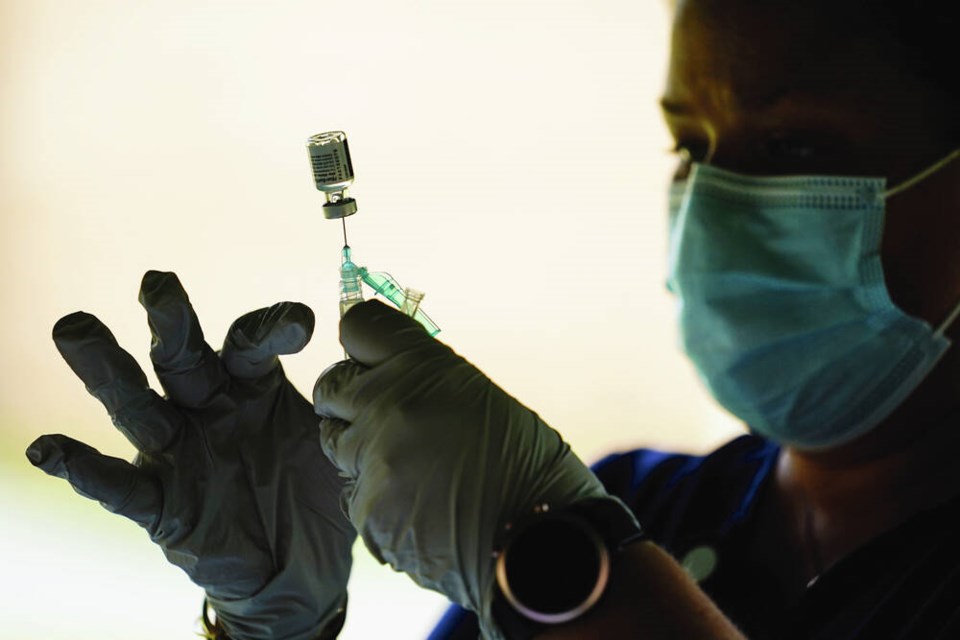
She didn’t want the vaccine. She talked about her exceptional immune system, her natural immunity, her great cardiovascular conditioning, all the vitamin D she took, and so on.
She said: “COVID is no worse than the flu. This is a big fuss about nothing.”
She is 70-something years old. She was also rushed to Emergency twice last summer, first for what turned out to be an allergic reaction and then for a worrisome combination of symptoms that was subsequently diagnosed as pneumonia and a blood clot in the lungs.
Then the government mandated vaccine passports for non-essential businesses and services, and started requiring people working in certain sectors and working with vulnerable people to be vaccinated.
If she wanted to continue her contract to teach yoga to fellow seniors at the local community centre, she was told, she had to provide proof of vaccination or a note from her physician stating she was medically exempt from the vaccination.
She visited her doctor.
She got her first shot the next day.
She is just one of the people getting their first shots since vaccine-passport requirements were announced. The “no jab: no job” approach has been overcoming hesitancy, reluctance and unwillingness among some who’ve been putting the vaccinations off.
Here, in B.C., the approach for most of 2021 has been gentle persuasion, repeated cajoling, and constant messaging. That worked for many people, most of whom just wanted to get back to life, work and activities as quickly as possible without putting themselves, their families, their coworkers or their clients or customers at unnecessary risk.
The pandemic has been costly. Entire sectors of the economy took hits. People have been out of work and, even now with employment rates improving, many people still work less than they did 20 months ago.
When business revenues and incomes fall, so do tax revenues.
And yet, during the past 18 months, governments have been increasing spending to help Canadians survive the crisis. They’ve provided recovery benefits and funding, subsidized new legislated sick leave, provided business relief grants, invested in housing options to keep vulnerable people on the street safer, funded research into the virus, etc.
How health-care dollars are spent has also changed, with vast amounts being redirected towards COVID-19 diagnosis, treatment, care, control, vaccination campaigns and contact tracing.
According to data from the Canadian Institute for Health Information, the average cost for patients treated for the virus is more than $23,000, four times higher than for a flu patient. However, for a COVID patient needing intensive care, the average cost more than doubles to more than $50,000 — about six times the cost of treating someone who’s had a heart attack.
The COVID-related healthcare spending surge in Canada could reach a record $308 billion in 2021, or roughly $8,019 per Canadian, according to CIHI projections.
Plenty of data from B.C. and elsewhere show that, since the summer, the majority of hospital and ICU cases continue to be people who weren’t vaccinated.
When COVID patients return home, many face many months of disability and rehabilitation for long COVID. They, too, draw on doctors, specialists, physiotherapists, occupational therapists and so on through their recovery. Some of those services are covered by MSP and some are paid for out of pocket, or, if you’re so privileged, are covered in part by private extended health-care insurance.
Private insurance companies are no doubt considering COVID’s costs to their bottom lines. Nobody should be surprised if whether COVID-19 vaccinations are up to date soon becomes a question on the application forms for extended health.
The companies may even raise premiums for people who are unvaccinated, just as they do for people who smoke. And the companies may also start screening new customers for past COVID illness — the complexity and variety of the long-term health effects that COVID has been shown to trigger could fall under “pre-existing conditions not covered.”
Then there are the delayed surgeries, the missed transplants, the interrupted or postponed chemotherapy, and so on. Those delays allow health conditions time to worsen. The costs of deferred treatment are social and economic.
As a society, as communities, as families and as individuals, we’ll be paying for the delays for years to come.
It’s no surprise then that governments have raised the stakes.
- - -
To comment on this article, email a letter to the editor: [email protected]