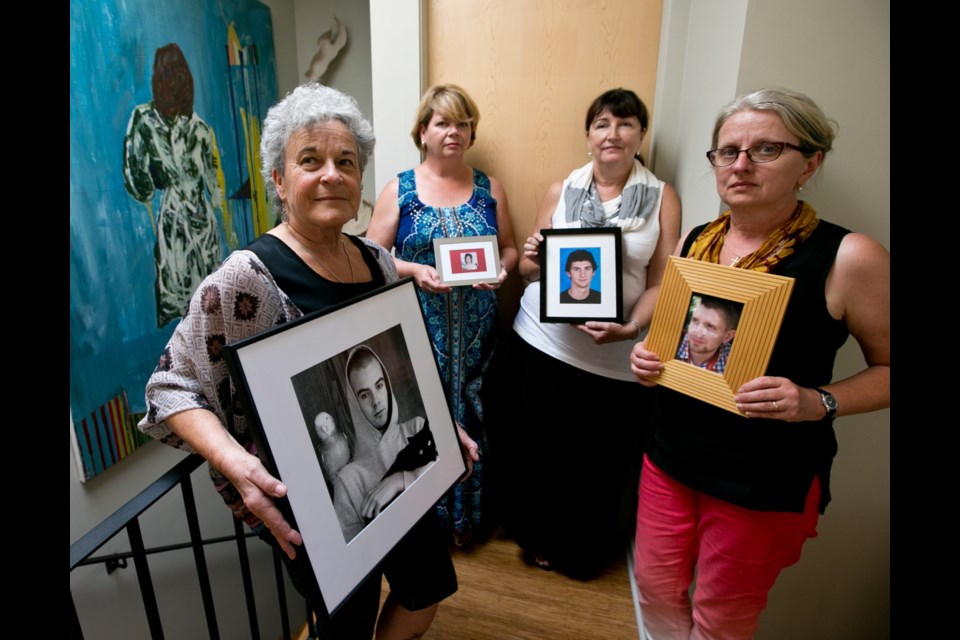A group of mothers who have lost adult children to drug addiction — sometimes by taking just one fentanyl pill — are pushing past their grief to mobilize changes in health policy they say could save many other lives.
Moms United and Mandated to Saving the lives of Drug Users, or mumsDU, kicked off a cross-Canada media campaign in Saanich last week, breaking the silence they say surrounds addiction-related deaths, on the rise due to the synthetic painkiller fentanyl, which is 50 to 100 times more potent than morphine.
The group says there is an urgent need to legislate easier access to naloxone, the drug antidote to fentanyl and other opioids such as morphine, heroin, methadone and oxycodone. Currently, a doctor’s prescription is required for the antidote, which can restore normal breathing after opioids have impaired respiration.
Health Canada recently acknowledged that naloxone has been used safely in Canadian hospitals for more than 40 years and plans to review broader access, but that would take 18 months or more.
“This is a death sentence for hundreds of people if they take 18 months,” said Leslie McBain of Pender Island.
McBain’s son, Jordan Miller, was 25 when he died in Victoria last year. He was found with many drugs in his system, but had been addicted to oxycodone.
“The numbers are changing every day because people are dying,” she said. “[Naloxone] is our first defence against deadly overdose.”
Fentanyl, used primarily to treat severe pain and available only by prescription in Canada, is a growing concern as the number of deaths and overdoses from the drug continue to climb.
There were at least 655 deaths in Canada involving fentanyl between 2009-2014, the Canadian Centre on Substance Abuse reports. There were a further 1,019 drug-poisoning deaths in which fentanyl was detected in post-mortem tests.
Anecdotal reports suggest that deaths and overdoses involving fentanyl occur in individuals who thought they were using heroin, oxycodone, cocaine or other drugs but mistakenly took fentanyl, according to the Canadian Community Epidemiology Network on Drug Use.
“When you’re dealing with a street drug, you have no idea how it has been made or what’s in it,” wrote Dr. Supriya Sharma and Dr. Gregory Taylor, Canada’s two top public health doctors, in a statement. The officials warned that fentanyl is “many times more powerful than other opioid drugs,” meaning even small amounts can lead to death.
B.C. is chief among provinces pushing for broader access to naloxone, with B.C. public health officials recommending the antidote be available behind pharmacy counters without doctors’ prescriptions, said Laura Heinze, spokeswoman for the Ministry of Health.
Since 2012, B.C. has distributed about 2,500 no-cost “take-home” naloxone kits to people who use opioids, and more than 4,000 people have been trained to administer naloxone, including users, their friends and families and health service providers, she said.
More than 250 overdoses have been reversed as a result.
Fentanyl on the Island: ‘We’re seeing it more and more’
In the first five months of 2015, there were 12 deaths on Vancouver Island in which fentanyl was found in the deceased, said Matt Brown of the B.C. Coroners Service.
Those include seven deaths in Nanaimo, two in Victoria, two in Campbell River, and one in Courtenay.
Accidental or undetermined deaths in illicit circumstances in which fentanyl was detected have increased seven-fold in B.C. from 13 deaths in 2012 to 90 deaths in 2014, the Canadian Centre on Substance Abuse said.
There have been trafficking charges laid but no large-scale seizures of fentanyl in Victoria, said Insp. Scott McGregor of the Victoria Police Department’s focused-enforcement team.
“We’re seeing it more and more compared to two years ago,” he said.